The mean insulin response curve (lower solid line) for the ITCVD group has greater values than the controls at all time intervals during the GTT with statistical significance at fasting (P < 0.05), two hours (P < 0.001) and three hours (P < 0.001). In addition, the insulin curve of the ITCVD group has a delayed peak at 2 hours. This means although OGTT is classified as normal, stroke pts have significantly higher insulin levels at fasting, 2 hr & 3 hr time points. If only 2 hr post glucose insulin were checked, hyperinsulinemia could be detected without doing the whole OGTT. It was around 80 microU/mL, so well over Kraft’s criteria of 40 microU/mL. On the other hand, if only OGTT were done without insulin assays, these abnormalities in CHO metabolism in 18 stroke pts would have been missed.
|
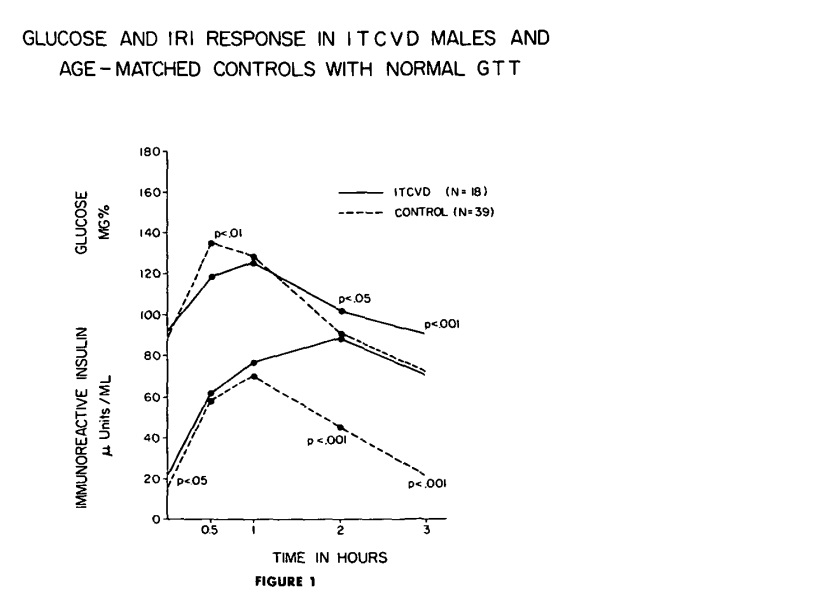
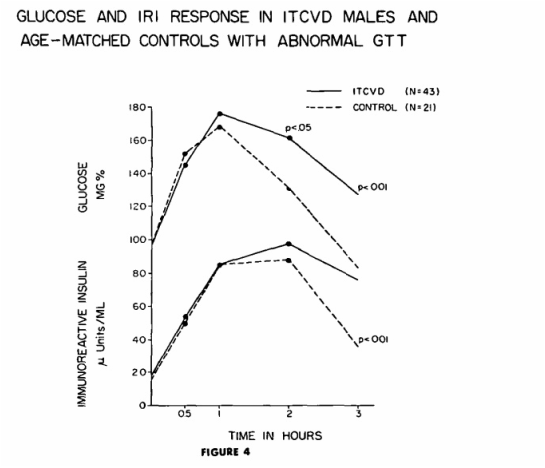
One more study (Stroke.1975;6(1):77-84.) supports Kraft’s statement that atherosclerotic diseases like AMI, Stroke, PAOD are hyperinsulinemic states. 61 ischemic thrombotic cardiovascular disease (ITCVD) patients and 61 age-matched control subjects were compared in order to detect risk factors for stroke. OGTT with insulin assays were done for all patients and controls. 18 ITCVD men and the 39 controls were classified as normal GTT. In fig 1, Glucose curve (upper solid line) of the ITCVD group peaks at one hour while the curve of the control group peaks at one-half hour, although both groups are classified as normal GTT. The mean insulin response curve (lower solid line) for the ITCVD group has greater values than the controls at all time intervals during the GTT with statistical significance at fasting (P < 0.05), two hours (P < 0.001) and three hours (P < 0.001). In addition, the insulin curve of the ITCVD group has a delayed peak at 2 hours. This means although OGTT is classified as normal, stroke pts have significantly higher insulin levels at fasting, 2 hr & 3 hr time points. If only 2 hr post glucose insulin were checked, hyperinsulinemia could be detected without doing the whole OGTT. It was around 80 microU/mL, so well over Kraft’s criteria of 40 microU/mL. On the other hand, if only OGTT were done without insulin assays, these abnormalities in CHO metabolism in 18 stroke pts would have been missed. 43 stroke patients and 21 control subjects were classified as abnormal GTT. In fig 4, it is obvious that 2 hr post glucose insulin level of both stroke and controls are around 80 microU/mL, so well over cutoff level of 40 microU/mL. These people (43+21) with abnormal CHO metabolism can be detected by OGTT without insulin assay.
0 評論
A large population study (n=2475) done in Israel showed insulin resistance is present in the great majority of hypertensive patients. 83.4% of the hypertensives were either glucose-intolerant or obese -- both established insulin-resistant conditions. Fasting and post-load insulin levels in a representative subgroup (n = 1,241) were significantly elevated in hypertension pts independent of obesity, glucose intolerance, age, and antihypertensive medications. This study was published in 1985! (J Clin Invest 1985;75:809)
In a series of 364 cerebrovascular disease patients admitted to Institute of Rehabilitation Medicine at New York University School of Medicine between 1965 and 1970, 281 were thrombotic, 41 were hemorrhagic and 42 were emboli. Of the 281 thrombotic stroke patients, OGTT with insulin assay was done only in 206 patients and 170 patients (82.5%) have overt T2DM or abnormal OGTT. OGTT was done in 20 hemorrhagic stroke patients and 19 (95%) of them showed abnormal OGTT or frank T2DM. Of the 22 emboli stroke patients, for which OGTT was done, 17 (77%) were either overt DM or abnormal OGTT. If Kraft's criteria were used, more patients would have been classified as Hyperinsulinemia/ T2DM.
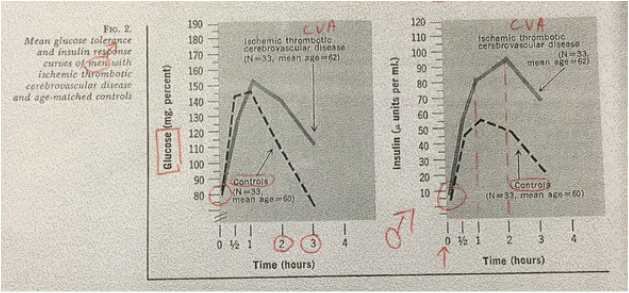
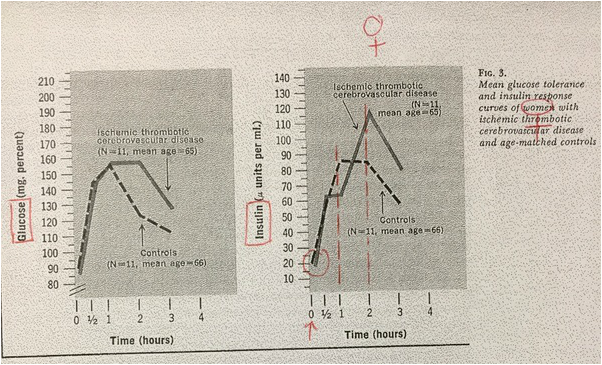
In figures 2 & 3, The mean fasting insulin levels are almost the same in men & women with ischemic trombotic CVA and their controls. However, mean insulin response of controls & diseased men and women are very different. Controls peak at 1 hr whereas thrombotic CVA patients (both men & women) peak at 2 hours (Kraft's pattern IIIA). This was published in 1972 (Geriatrics 1972;27:105-116) & clearly showed that stroke is also a hyperinsulinemic state / type 2 DM either overt or in situ. The following is extract from the article "Insulin and Atheroma" by Dr Robert W. Stout:
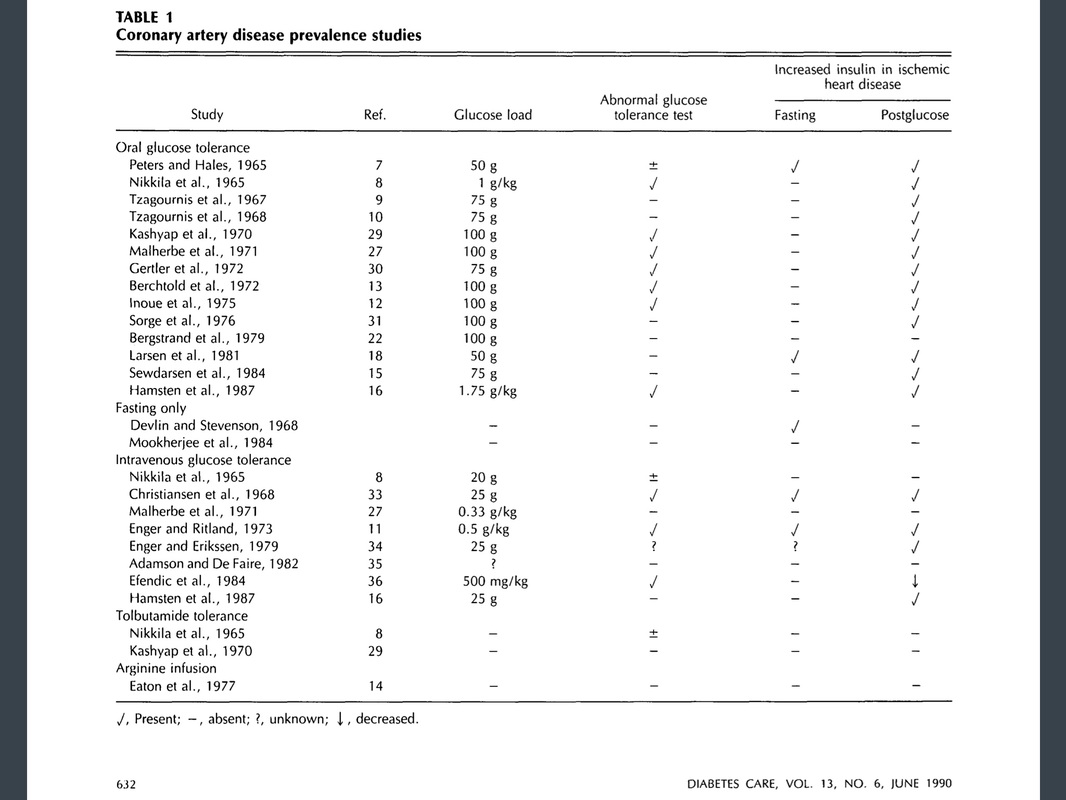
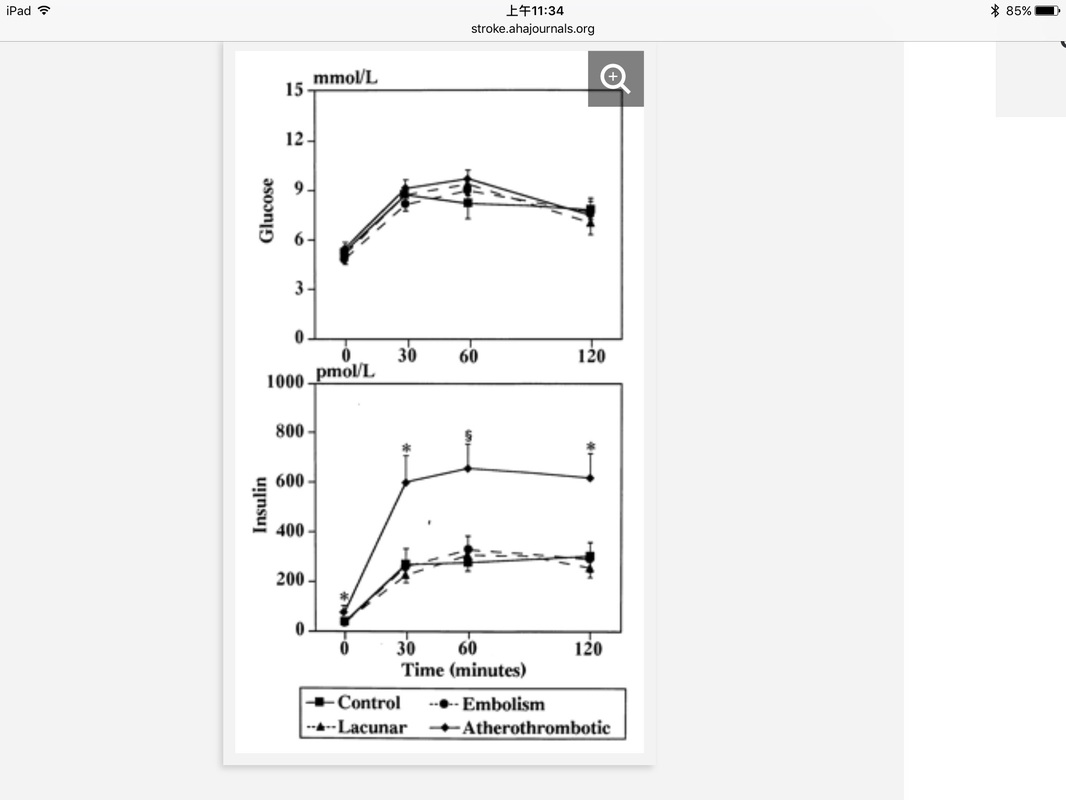
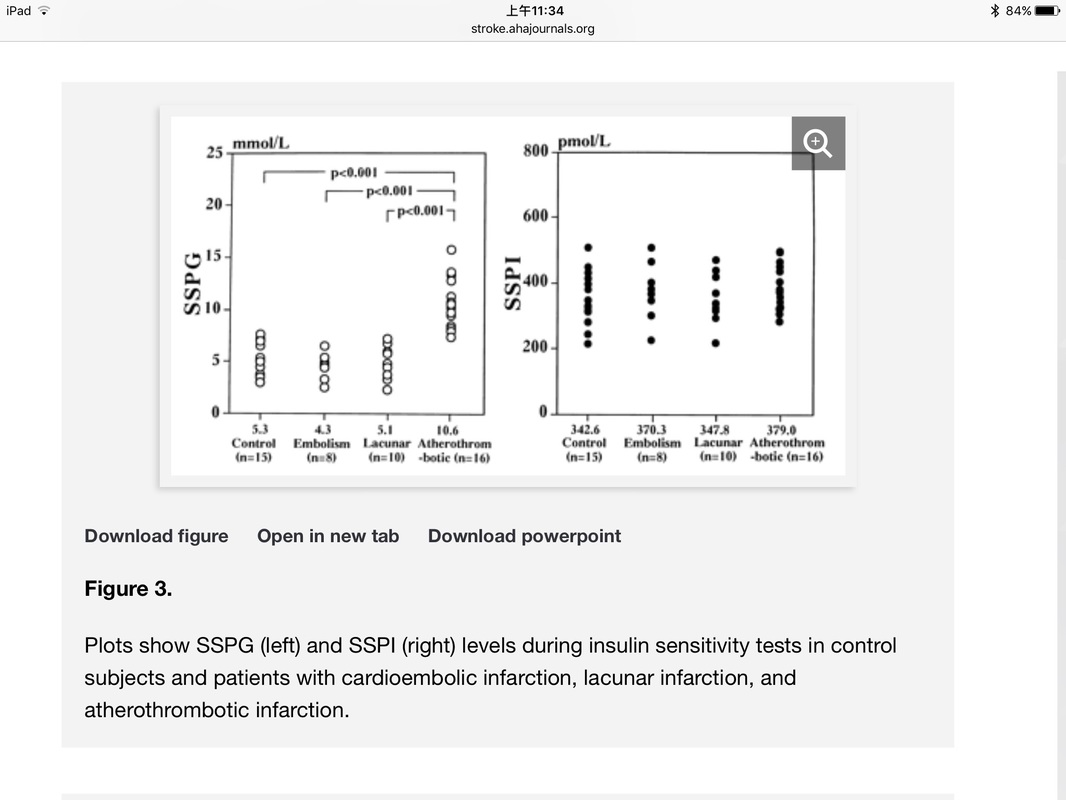
The overwhelming mass of evidence favors an increased insulin response to oral glucose in patients with ischemia of the heart, lower limbs, or brain. Table 1 from this article is shown below: I found one Japanese study in "Stroke" journal published in 1996. It's actually a combination of Kraft's OGT(+ insulin) and Reaven's insulin-mediated glucose uptake assessment (insulin suppression test) in ischemic stroke pts (16 atherothrombotic infarction; 10 lacunar infarction; 8 cardioembolic infarction) and 15 control subjects. After 75g glucose ingestion, glucose responses in all 4 groups were the same (Fig 1, top graph). This means OGT with glucose assay only is unable to detect any difference between 4 groups. However, if insulin assay was added (as Kraft did), insulin responses (at 30, 60 & 120 min) were significantly higher in pts with atherothrombotic infarction compared with other 3 groups (Fig 1, bottom graph). Insulin sensitivity was assessed by so-called insulin suppression test. Endogenous insulin was suppressed with Sandostatin IV infusion. Glucose & insulin were infused IV until a steady state was reached at 2 hrs. In fig 3, right SSPI (steady state plasma insulin) in all 4 groups were kept about the same. Therefore, the SSPG (steady state plasma glucose) on the left reflects relative insulin sensitivity of the 4 groups. SSPG of atherothrombotic infarction pts were significantly higher than the other 3 groups, which means at approximately the same level of insulin, cells of atherothrombotic infarction pts were resistant to insulin action compared with the other 3 groups. No wonder my favorite study showed all CVA cases ocurred in most insulin resistant & moderately resistant persons. Nobody in the most insulin-sensitive tertile had any CVA.
So, my conclusion is atherothrombotic cerebral infarction is an insulin resistant state, just like hypertension, T2DM & obesity. They selected non-obese, non-diabetic & non-hypertensive stroke pts in this study, so insulin resistance appears to be the important determinant of atherosclerosis. The answer is yes!!
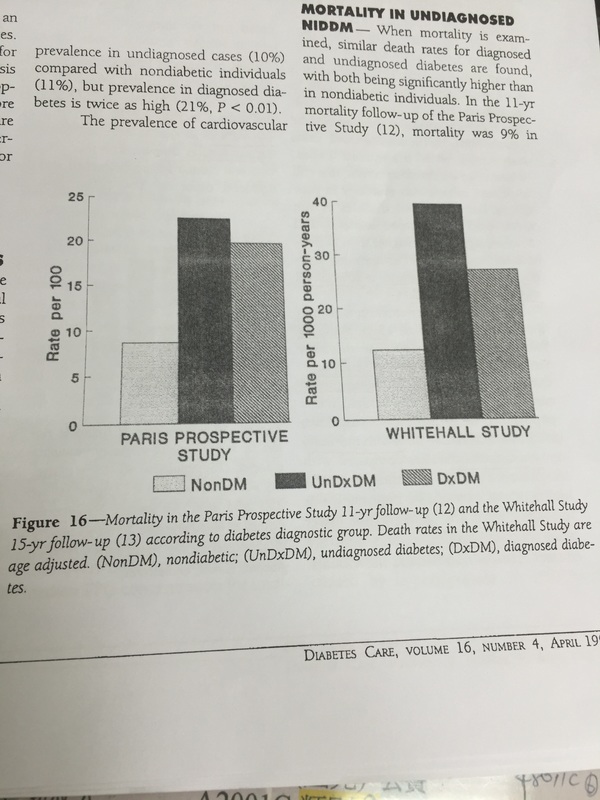
Fasting insulin > 30 microU/mL (upper limit of normal) is hyperinsulinemia / T2DM. However, Kraft's cumulative study of 14,384 OGTT with insulin assays showed that < 8% of those with hyperinsulinemia / T2DM have fasting insulin > 30 microU/mL. If fasting insulin of >30 microU/mL were used as cutoff for T2DM diagnosis, 92% T2DM cases would be missed. Therefore, 2 hr post 75g glucose insulin level is more sensitive in detecting early T2DM. Onset of NIDDM probably occurs at least 12 yrs before its clinical diagnosis. 21% of newly diagnosed pts have retinopathy. Undiagnosed NIDDM is not a benign condition. The prevalence of macrovascular disease in undiagnosed NIDDM is about equal to that found in diagnosed DM, & rates of CHD in both diagnosed and undiagnosed DM are about twice that for nondiabetic individuals. Mortality in undiagnosed DM is also equal to that of diagnosed DM, and both are significantly higher than in nondiabetic individuals.
In both Paris Prospective study and Whitehall Study, as shown below, mortality in undiagnosed as well as diagnosed DM pts is more than 2 fold that of nondiabetic persons. Therefore, it is clear that undiagnosed DM is as deadly as diagnosed DM. Kraft's OGT with insulin assay can capture earliest DM (ie. DM in situ), at least 10 yrs earlier than fasting glucose or routine OGTT which measures glucose only. In Dr. Kraft's 14,384 oral glucose tolerances with insulin assays, there were 5,128 or 35.6% with glucose levels < 60 mg/dl (hypoglycemia) after the 1st hour peak. 3790 or 74% of the 5,128 were hyperinsulinemia, type 2 DM. What's more interesting is 2532 or 49% of 5128 hypoglycemic persons showed normal glucose tolerance which means they would be regarded as normal by OGT, but Kraft's criteria put them in hyperinsulinemia type 2 DM category! Hypoglycemia associated with hyperinsulinemia type 2 DM is designated functional hypoglycemia. Postprandial hypoglycemia is an indication for identification or exclusion of hyperinsulinemia type 2 DM by OGT with insulin assay. Hypoglycemia causes drowsiness following meals, lasting about 30 minutes during which driving is dangerous and reading almost impossible.
It is noteworthy that insulin's actions include skeletal muscle vasodilation via an increase in EDNO(endothelium-derived nitric oxide)which can inhibit vascular smooth muscle proliferation, reduce platelet adhesiveness & decrease lipid peroxidation, actions which have the net effect to reduce atherosclerosis progression. In insulin-resistant obese persons, endothelium-dependent vasodilation is reduced by 40-50% compared to lean persons. This is shown in an exellent article.
In one of Kraft's articles (1995), there is a table showing summary of insulin levels for detection of T2DM in situ. Click here to view article.
|
Archives
七月 2021
Categories |

 RSS 訂閱
RSS 訂閱
