Despite all these giant high quality studies published in peer-reviewed medical journals, the expert organizations keep on singing the old song of low fat diet with saturated fat less than 10% of total calorie. Old dogmas die hard and we must keep on fighting outdated guidelines from organizations with huge conflicts of interest.
|
PURE study is an international prospective epidemiolgy study involving 18 countries with a median follow-up of 7·4 years. Just as in Women's Health Initiative which is another huge study showing low fat diet fails, PURE study shows once again that intake of total fat and each type of fat was associated with lower risk of total mortality (quintile 5 vs quintile 1, total fat: HR 0·77 [95% CI 0·67-0·87], ptrend<0·0001; saturated fat, HR 0·86 [0·76-0·99], ptrend=0·0088; monounsaturated fat: HR 0·81 [0·71-0·92], p trend<0·0001; and polyunsaturated fat: HR 0·80 [0·71-0·89], p trend<0·0001). Higher saturated fat intake was associated with lower risk of stroke (quintile 5 vs quintile 1, HR 0·79 [95% CI 0·64-0·98], p trend=0·0498). Total fat and saturated and unsaturated fats were not significantly associated with risk of myocardial infarction or cardiovascular disease mortality. This is totally in contrast to Ancel Key's Seven country study which started the low-fat mania 3 decades ago.
Despite all these giant high quality studies published in peer-reviewed medical journals, the expert organizations keep on singing the old song of low fat diet with saturated fat less than 10% of total calorie. Old dogmas die hard and we must keep on fighting outdated guidelines from organizations with huge conflicts of interest.
0 評論
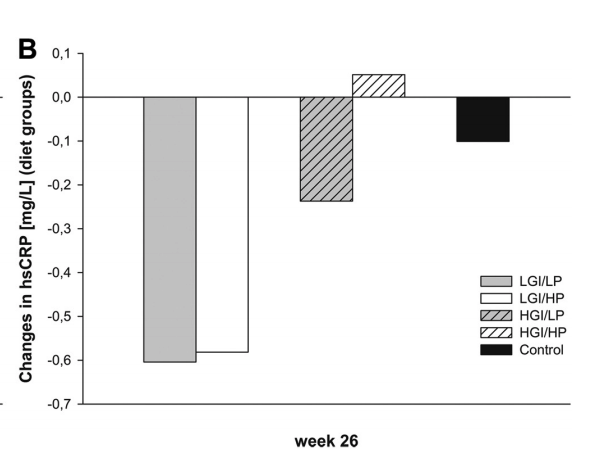
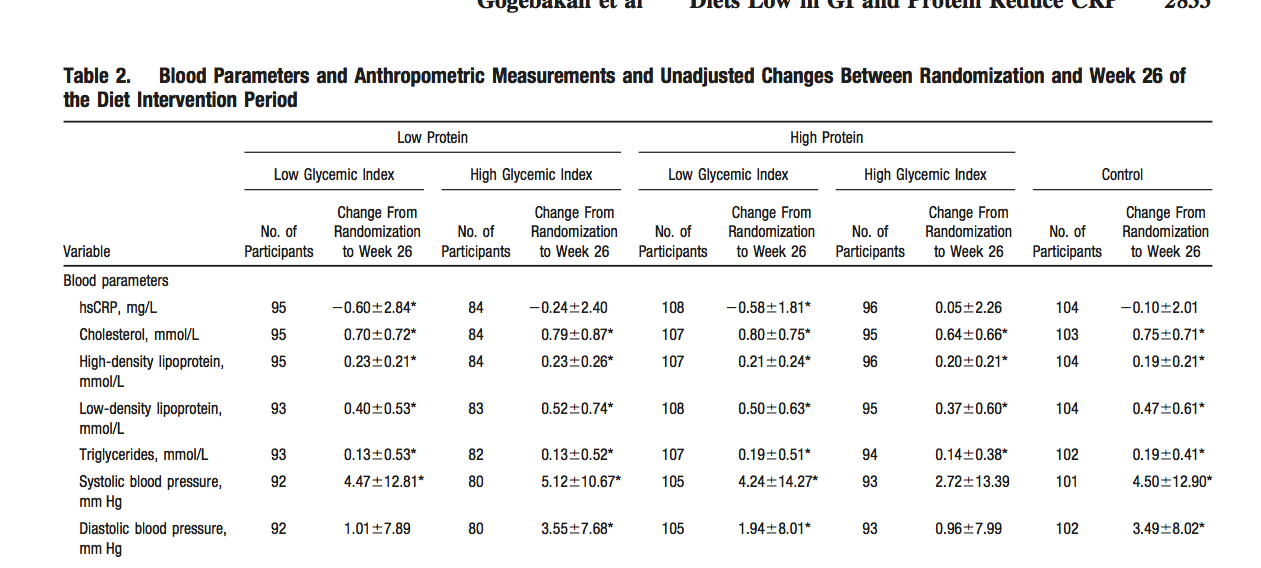
A relatively large study (N=773) done in Europe gives clues to answer the above question. This study is called DiOGenes(Diet, Obesity and Genes study), which is a Randominzed Controlled Trial involving volunteers from 8 European countries. There are 2 parts in this study: 1st part is weight loss phase during which volunteers ate low-calorie diets for 8 weeks and lost weight; 2nd part is weight maintenance phase during which subjects were randomized to 1 of 5 ad libitum diets for 26 weeks. These 5 were (1)Low protein, low glycemic index [GI];
(2) Low protein, high GI; (3)High protein, low GI; (4)High protein high GI; (5)Control diet [according to national dietary guidelines]. Their hsCRP levels were compared in the following figure which shows only low GI groups (whether low protein or high protein) have significant reduction in hsCPR levels (P<0.05). The 2 high GI groups (both low protein and high protein) and control group had changes that were statistically non-significant (P>0.05). This might be related to expected reductions of postprandial glucose levels with low-glycemic-index diets, with glucose known to stimulate the expression of inflammatory genes by epigenetic mechanisms. Furthermore, transient increases in glucose induce persistent changes in histone methylation patterns at promoters of inflammatory genes, which is related to glucose-induced mitochondrial generation of oxygen radicals. Long-term increases in basal glucose concentrations are associated with both high fasting insulin concentrations and insulin resistance, which is known to promote inflammatory processes and an increment of hsCRP. According to Dr. Steven Gundry, all autoimmune diseases are caused by alterations in the good bugs and the bad bugs that live in our gut, our mouth and on our skin (known as microbiome), along with a change in the permeability of our gut wall (aka leaky gut).
What impacts that permeability? NSAIDs, antibiotics, acid-blocking drugs such as Nexium and pesticide Roundup all change our gut flora and the mucous layer of our gut. This compromises the barrier of our intestines on a daily basis, thereby allowing lectins in. Copious research over the last half century reveals that gulping down NSAIDs is like swallowing a live grenade. These drugs blow gaping holes in the mucus-lined intestinal barrier. As a result, lectins, LPSs, & living bacteria are able to deluge the breaks in your gut, flooding your body with foreign invaders. And this confluence of forces prompts our immune system to unleash an attack on ourselves, in a classic case of mistaken identity caused by molecular mimicry. In fact, much of what we assume as a normal part of the aging process is actually the cumulative effect of Lectin toxicity. Ref: Plant Paradox by Steven Gundry Growing number of studies from top milk-producing countries like Australia, New Zealand, and some European nations enumerate the benefits of A2 milk and the health risks associated with continuous consumption of A1 milk.
In his book called Plant Paradox, Dr Gundry from the US explained like this: about 2000 years ago, a spontaneous mutation in Northern European cows caused them to make the protein casein A–1 in their milk instead of the normal casein A-2. During digestion, casein A-1 is turned into a lectinlike protein called beta-casomorphine. This protein attaches to the pancreas's insulin-producing beta cells, which prompts an immune attack on the pancreas of people who consume milk from these cows or cheeses made from it. I could not believe what I saw, so searched pub med & sure enough I found the following: Type I (insulin-dependent) diabetes mellitus and cow milk: casein variant consumption. An extract from this 1999 paper says: The A1 and B variants of beta-casein have a histidine at position 67 that determines the enzymatic cleavage of the molecules yielding beta-casomorphin 7. The A2 variant does not cleave at this position due to the presence of a different amino-acid (proline). Beta-casomorphin-7 has opioid properties, and has been shown to inhibit human intestinal lymphocyte proliferation in vitro. It is possible that such an immune suppressant influences the development of gut-associated immune tolerance, or suppresses defence mechanisms towards enteroviruses, both of which have been implicated in the aetiology of Type I diabetes. Other immunosuppressive effects which might contribute to diabetes include activation of endogenous retroviruses associated with the disease. Click the link below to see full abstract on medline: https://www.ncbi.nlm.nih.gov/pubmed/10096780 Another paper included even IHD. Holy shit! Look below: Ischaemic heart disease, Type 1 diabetes, and cow milk A1 beta-casein. https://www.ncbi.nlm.nih.gov/pubmed/12601419 According to New Zealand research conducted by CN McLachlan, the regular intake of common milk containing A1 beta-casein inspires the development of coronary heart disease. Click the link below for full abstract: https://www.ncbi.nlm.nih.gov/pubmed/11425301 Luckily this is still controversial. That said, Dr Gundry's case reports showed that in susceptible persons, different breeds provoke different responses. The following is a website providing information about A1 & A2 difference: https://www.authoritydiet.com/a1-vs-a2-cows-milk-what-difference-benefits-nutrition/ The following was extracted from RD:
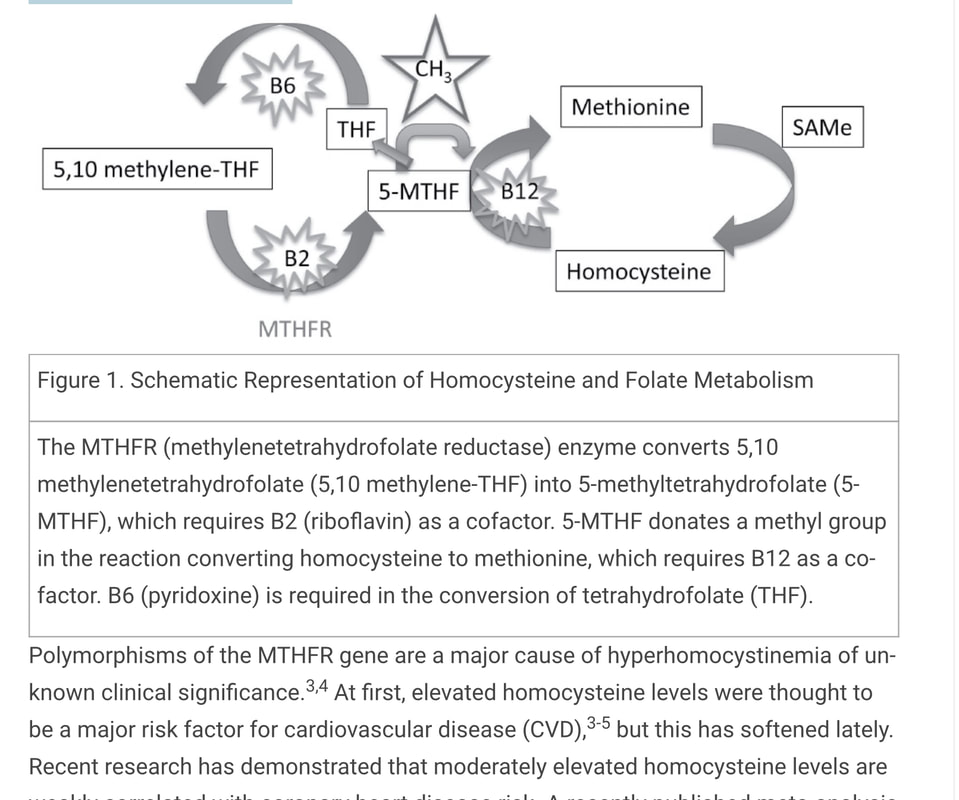
Low-carb diets have been around for years, but adding healthy fat is the new twist. Fats from dairy, nuts, fish and eggs (including the yolk) are healthy, whereas overconsumption of vegetable oils and trans fats can lead to chronic disease. A growing body of evidence shows our 30-year message to avoid fat has been misguided and fat instead is satiating, good for the heart and brain, and, compared to other food groups, has the least impact on insulin release. Swedish diabetes researcher and head of internal medicine at Linkoping University Dr. Fredrik Nystrom agrees. His dietary advice: “Carbohydrate restriction in combination with the high fat Mediterranean diet [fish, some meat, vegetables, cheese, nuts, olive oil]". Click the link below to see the whole article https://www.rd.com/health/conditions/how-to-avoid-becoming-diabetic/ Methylenetetrahydrofolate reductase (MTHFR) is a key regulatory enzyme in folate & homocysteine metabolism. MTHFR is also acronym for the gene that encodes this enzyme. MTHFR enzyme deficiency can cause hyperhomocysteinemia. Currently, 34 rare but deleterious mutations in MTHFR gene, & 9 common variants (polymorphisms) have been reported. The 677C→T (A222V) variant is the most common genetic cause of hyperhomocysteinemia. The disruption of homocysteine metabolism by this polymorphism influences risk for several complex disorders. Mental health issues, such as depression, bipolar disorder, schizophrenia, ADHD, or autism are linked to having an MTHFR mutation. MTHFR mutations also increase the risk of CVD and stroke, recurrent early miscarriage, migraine with aura, osteoporosis, and some cancers.
Mudd et al 1st identified a patient with homocystinuria due to a severe deficiency of the MTHFR enzyme. This type of deficiency is relatively rare. In 1988, a thermolabile variant of MTHFR enzyme was identified in patients with cardiovascular disease. With the identification of a MTHFR polymorphism (i.e., a common mutation) that results in mild hyperhomocysteinemia, it became clear that some diseases of adulthood, such as CVD, reflect milder versions of the fulminant biochemical defect present in the newborn or child with severe MTHFR deficiency. This milder deficiency, which appeared to be more common, resulted in a mild to moderate elevation of plasma total homocysteine, an emerging risk factor for cardiovascular disease. The 2 most common polymorphic variants that affect enzyme activity are the C677T & the A1298C variants. Because there are 2 copies of each gene, an individual can be homozygous for the C677T variant. This can cause hyperhomocysteinemia if the individual also has a low plasma folate. Individuals who are heterozygous for C677T have one copy of the C677T variant and one "wild type" or normal copy. These C677T heterozygous individuals do not demonstrate elevated homocysteine. C677T homozygous variant enzyme is thermolabile and demonstrates 70% reduced enzyme activity in vitro. The heterozygous C677T MTHFR enzyme has 35% reduced activity in vitro. It is estimated that 32% of Mexicans, 10-15% of North American Caucasians, and 6% of people of African descent are C677T homozygous. An Italian study investigating forms of folate (dietary, 5-MTHF, and folic acid) & effect on total plasma homocysteine levels found that all 3 experimental groups had lowered plasma homocysteine levels compared to the controls. The study showed that a folic acid-enriched food diet (400 µg/day), supplemental folate in the form of 5-MTHF (200 µg/day), and folic acid (200 µg/day) are comparable in reducing total homocysteine levels irrespective of MTHFR genotype status. For further details click the following links: https://www.reliasmedia.com/articles/115810-mthfr-clinical-considerations-a-review https://www.omicsonline.org/open-access/clinical-implications-of-mthfr-gene-polymorphism-in-various-diseases-0974-8369.s3-e101.pdf The advent of the agricultural revolution about 10,000 years ago meant that a totally new source of food – grain and beans – became the dietary staple relatively quickly. Until then, the human microbiome had never encountered lectins in grains or legumes, and therefore the human gut bacteria and immune system had zero experience handling them.
We can see that lectins in oats, grains & legumes have always been toxic. But given the choice between starvation & some serious health trade-offs, humans will always opt for survival. Without grains & beans, civilization would not have occurred. Plants attack your defense system with their own three-pronged approach, making you feel sick on several fronts. Strategy # 1: The first mission of lectins is to pry apart tight junctions between enterocytes. Normally lectins should not be able to squeeze past the mucosal cells. But if your defense lines are breached, lectins can pry apart tight junctions by binding with receptors on certain cells to produce Zonulin. Zonulin opens up the spaces between enterocytes, which enables lectins to access the surrounding tissues, lymph nodes, or bloodstream. Once there, they act like any foreign protein, prompting your immune system to attack them. Strategy #2: Plants purposely make lectins that are virtually indistinguishable from other proteins in your body, a tactic called molecular mimicry. By mimicking human proteins, lectins fool the host’s immune system, causing it to attack the body’s own proteins. Multiple studies of arthritic patients have demonstrated elevated antibody levels for gliadin which is the principal component of wheat gluten. Gluten-free diets have been shown to be effective in reducing arthritic symptoms in celiac patients. Strategy #3: Lectins can bind to important receptors on the cell walls, either giving wrong information or blocking release of the correct information. For example, the lectin WGA bears a striking resemblance to insulin. It can attach to insulin receptor as if it were the actual insulin molecule, but unlike the real hormone, it never lets go – with devastating results, including reduced muscle mass, starved brain cells, and plenty of fat. Gluten, the protein found in wheat, barley,rye, and often oats, is just one form of lectin. All gluten foods contain lectins. Almost all grains & pseudo-grains contain glutenlike lectins. So-called gluten-free products are actually full of lectins in the form of flours made from corn, oats, buckwheat, quinoa,and other grains & pseudo-grains, as well as soybeans & other legumes. Wheat germ agglutinin (WGA) is found in Bran. This means that white bread contains gluten but not WGA, while whole wheat bread contains both. WGA is a small protein compared with most other lectins. So even if the gut mucosal barrier has not been compromised, WGA can pass through the walls of intestine more easily than other lectins can. WGA also:
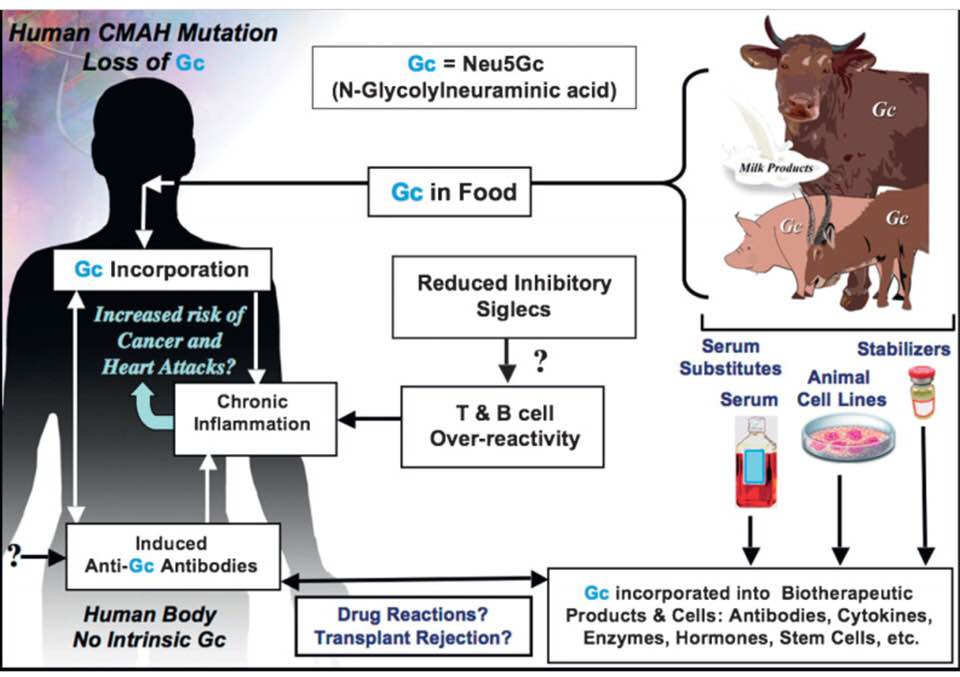 Scary, but we must face the science which shows non-human sugars (Neu5Gc) from meat & dairy are incorporated into human cell surfaces. Our immune system detects these foreign sugars & produce antibodies to attack them. This evokes inflammation in our blood vessels & could lead to heart disease. Sialic acids are monosaccharides (sugars) typically found at the outer ends of glycan chains (glycoconjugates aka glycocalyx) covering the surface of all vertebrate cells. The most commonly expressed sialic acid is N-acetylneuraminic acid (Neu5Ac), which is the precursor for N-glycolylneuraminic acid (Neu5Gc) synthesis, via action of the CMP-N-acetylneuraminic acid hydroxylase (CMAH) enzyme. Humans lost the ability to make Neu5Gc at the time our species diverged from chimps & gorillas 8 (2-3 in another paper) million years ago. Instead humans make Neu5Ac, as do elephants, chickens & shellfish. Although Neu5Gc is foreign to humans, our intracellular biochemical pathways cannot distinguish between Neu5Ac and Neu5Gc, which differ by one oxygen atom. Thus, exogenous Neu5Gc is taken up and metabolically incorporated into human cells, eventually being expressed on the cell surface as if it were made in the same cell. Furthermore, orally ingested Neu5Gc is taken up into the human body, & small amounts of Neu5Gc are present in normal human tissues. Interestingly, the Neu5Gc-rich foods identified to date are red meats, which have been associated with circulating inflammatory markers indicating endothelial dysfunction. Although Neu5Ac and Neu5Gc seem biochemically indistinguishable to human intracellular biosynthetic pathways, the latter is immunogenic in humans, leading to anti-Neu5Gc–specific antibody responses. Although such antibodies had been reported in some diseases, it was only recently recognized that all adult humans express them. Indeed, normal humans can express high titers of circulating anti-Neu5Gc immunoglobulin IgG & IgM antibodies against a variety of Neu5Gc-containing epitopes commonly found on endothelial cells. These data indicate a novel human-specific mechanism in which Neu5Gc-rich foods deliver immunogenic Neu5Gc to the endothelium, giving anti-Neu5Gc antibody- and complement-dependent activation, and potentially contributing to human vascular pathologies. In the case of atherosclerosis, Neu5Gc is present both in endothelium overlying plaques and in subendothelial regions, providing multiple pathways for accelerating inflammation in this disease. For further details, click the following link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2792214/ A lovely human and humane documentary out of Australia called "The Magic Pill" has been available on Netflix. We should have mentioned it earlier, but better now than to have forgotten completely.
The idea for the film was conceived by Pete Evans, a famous chef in Australia and photographed beatifully by Rob Tate with a compelling story to tell. The documentary is about food, and particularly how the Western diet has sabotaged the health of so many people. Some of those featured include Aboriginal peoples who 70 years ago were slender, fit and healthy (photos provided) but who have since succumbed to diseases of civilization, notably obesity and type 2 diabetes. In "The Magic Pill" their story is documented and shown cinematically over a period of time as they are provided low carbohydrate ketogenic foods and discuss on camera how they feel on this new diet. Other people are also featured, including a family with an autistic son, who's improvement on a ketogenic diet is also documented. While cancer is not the focus of the film, the filmmakers interviewed Gene to discuss cancer and ketogenic diets. The spot is only about 2 minutes long, and while not the highlight of the film, you may be interested to watch. One disease, one cause, many symptoms.
Reaven’s problem was like that faced by Dawin & Galileo, who’s findings estranged them from religious orthodoxy. Reaven’s unifying hypothesis of chronic disease not only offends his colleagues in cardiology; it strikes at the very heart of “pharmacological model” practiced in modern medicine. If obesity, diabetes, heart disease, NAFLD (Non alcoholic fatty liver disease), high blood pressure, & perhaps even cancer & dementia are, in fact, all symptoms of the same underlying condition – Insulin Resistance – then our current model of medical management must be wrong, requiring as it does, specific but different pharmacological treatments for each separate condition overseen by different hierarchies of medical specialists. And what if the cornerstone for treatment of all these conditions is a low carbohydrate diet, the very diet that has been vilified by Tim’s profession for the past 50 years? |
Archives
七月 2021
Categories |
 RSS 訂閱
RSS 訂閱
